If one day, replacing missing teeth no longer required drilling bones or inserting screws (dental implants), but simply a shot to grow your own “real teeth,” how long would you be willing to wait?
This is not a science fiction movie, but reality happening right now. Kyoto University in Japan and the startup company Toregem Biopharma are working on developing the world’s first **“tooth regeneration drug.”** This technology is seen as the long-awaited **“third set of teeth”** for humanity, following baby teeth and permanent teeth.
This article will avoid complex academic jargon and explain in detail the underlying logic of this technology, its current progress, and how it compares to existing dental implant methods.
I. The core of the technology: Why can’t humans replace their teeth like sharks?
To understand this Japanese technology, we first need to dispel a myth: in fact, human gums always contain **“tooth seeds”** (tooth buds).
Sharks and crocodiles can replace their teeth indefinitely, but once humans get permanent teeth, this ability seems to “turn off.” Professor Katsu Takahashi’s team at Kyoto University discovered that the key to this “switch” lies in a protein called **USAG-1**.
1. USAG-1: The “brake” that stops tooth growth
Research shows that the USAG-1 protein inhibits tooth growth. This mechanism was originally designed to prevent people from having too many teeth (polyodontia), but when teeth are missing, it becomes a barrier instead.
- The principle behind this Japanese technology: They developed a **“neutralizing antibody drug”** that can temporarily block the function of USAG-1.
- For a simple analogy: Your gums are like a car that wants to move forward, but USAG-1 keeps stepping on the brakes. This drug removes those brakes, allowing the dormant “tooth buds” to restart and develop into a complete tooth.
2. From mice to ferrets: Success stories
Early animal experiments were quite remarkable. After injecting the drug into mice and ferrets (whose tooth structure is similar to that of humans), new teeth were successfully induced, and these teeth had normal shapes and arrangements.
II. Timeline: How much longer do we have to wait? (2024-2030)
This is the question that all patients care most about. According to the official timeline released by Toregem Biopharma, progress is going better than expected, but we are still some way away from widespread availability.
- September 2024 (Milestone): Phase I clinical trials officially begin at Kyoto University Hospital in Japan.
Par
- ticipants: Healthy men aged 30 to 64 who are missing teeth.
Objective:
- To determine the safety of the drug in humans (will there be any side effects? Will it cause abnormal growth of other bones in the body?).
- ticipants: Healthy men aged 30 to 64 who are missing teeth.
- 2025 – 2026 (Estimat
- ed): Phase II clinical trials will begin.
- 2030 (Ultimate goal): If everything goes well, the drug wil
- l be officially approved for ma
- rket release.
Initial use: For patients with congenital tooth loss.
III. Comparison: Regenerated teeth vs. dental implants
Currently, the gold standard in dentistry is “dental implants.” So, what exactly are the advantages of Japan’s regenerative tooth technology compared to implants? It’s not just a matter of “real” versus “fake.”
| Comparative dimensions | Japan’s tooth regeneration technology | Traditional dental implants |
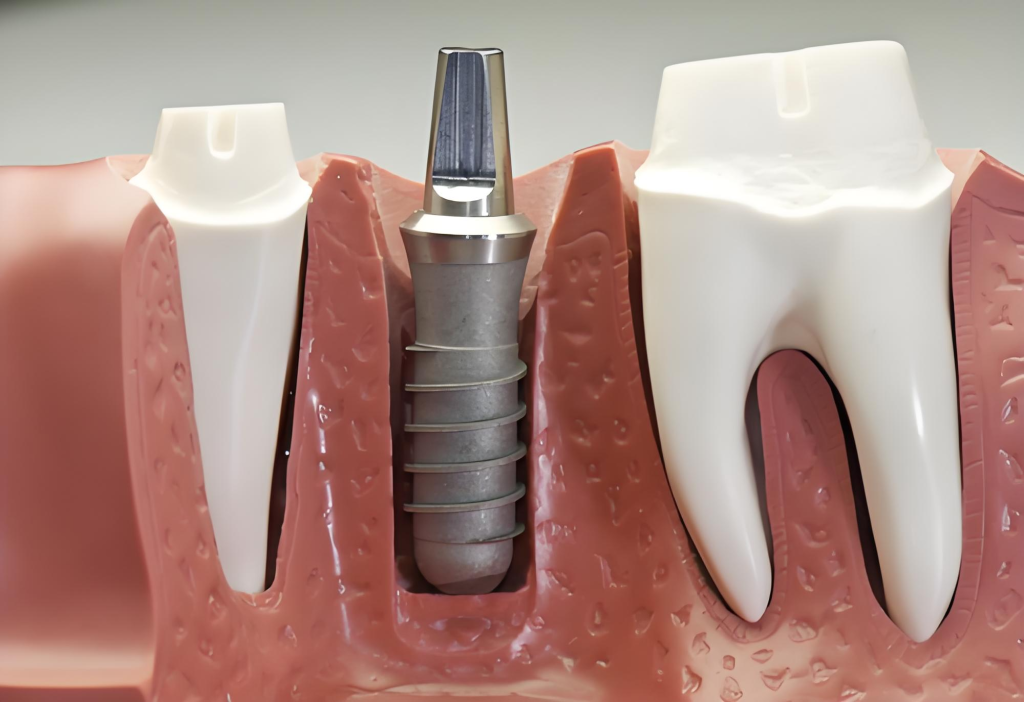
| Core structure | Features a “periodontal ligament” | Titanium fuses directly with bone (osseointegration) |
| Biting sensation | Provides cushioning and sensation, allowing precise detection of food texture | Hard contact; lacks neural feedback, resulting in a slightly duller biting sensation |
| Corrective capabilities | Once they have grown in, their position can be adjusted by wearing braces | Once implanted, their position remains permanent and cannot be changed |
| Surgical risks | Minimally invasive (intravenous injection), no need to cut into the gum tissue | Involves drilling, with risks of infection and nerve damage |
| Difficulties in maintenance | Just like natural teeth (can get cavities, suffer from periodontal disease) | Don’t get cavities, but may develop “peri-implantitis” |
💡 Key difference: The periodontal ligament (PDL)
This is
the greatest advantage of regenerative teeth. The periodontal ligament acts as both a “shock absorber” and a “sensor” between the tooth root and the bone. The reason why dental implants feel “stiff” when biting is precisely because they lack this ligament. Regenerative teeth allow you to regain the pleasure of chewing.
IV. Finding New Approaches: Currently Used “Pulp Regeneration” Technologies
Aside from “growing new teeth,” Japan is also at the forefront of the world in “saving damaged teeth.” These technologies have actually already been applied clinically, but they are not widely known.
This is what “pulp stem cell regeneration therapy” entails.
- The problem: In the past, when the dental nerve died (due to periapical periodontitis), the only option was “root canal treatment,” which involved removing the nerve. As a result, the tooth became dead, becoming brittle and darker in color.
- New technology: Some clinics in Japan, such as RD Dental Clinic, use the patient’s own stem cells—usually obtained from wisdom teeth or deciduous teeth—to cultivate them and then inject them into the hollowed-out pulp chamber.
- Result: The nerve and blood vessels can regrow! The tooth regain sensation and nutritional supply, significantly extending its lifespan.
- Current status: This technology has been approved by Japan’s Ministry of Health, Labour and Welfare for clinical use. Although it is expensive (around several hundred thousand yen per tooth), it offers new hope for patients who do not want to have their teeth extracted.
V. A Rational Note of Caution: Practical Challenges
Despite the promising prospects, as a rational observer, it is important to highlight the following potential pitfalls:
- Price Barrier: Given the regulatory patterns for biologics, it is highly likely that by early 2030, the cost of this “tooth-growth injection” will be much higher than that of dental implants. It may become a luxury available only to the wealthy or limited to patients with specific medical conditions covered by insurance.
- Shape Control: Naturally grown teeth have uncontrollable shapes and positions. Will the newly grown tooth be straight or misaligned? This suggests that **“regenerative medicine + orthodontics”** might become the standard approach in the future, with a treatment duration significantly longer than that of dental implants (about 3–6 months) – possibly taking 1–2 years.
- Safety Concerns: Could blocking USAG-1 lead to increased bone growth in other parts of the body? Long-term monitoring of data will be necessary to determine this.
Japan’s dental regeneration technology is ushering dentistry into a new era, moving it beyond “restorative engineering” (fillings, implants) towards “regenerative medicine”.
For patients who currently lack teeth, it is not advisable to wait until 2030. The bone loss caused by missing teeth is irreversible, and prolonged toothlessness can lead to facial deformities and adjacent teeth shifting. At present, high-quality dental implants (such as those from Korean or European brands mentioned earlier) remain the most reliable solution.
However, for younger generations or children with congenital tooth deficiencies, the future indeed holds promise. Perhaps one day, our grandchildren will ask, “Grandpa, what are dentures?”